Frozen shoulderA condition where shoulder movement becomes very limited and painful. The cause is often unknown, bu More, also known as adhesive capsulitis, is a condition that causes pain and then progressive stiffness in the shoulder jointThe glenohumeral joint is a ball-and-socket synovial joint and is the most mobile joint in the human More so that it eventually becomes “frozen” and almost immovable. No precise cause has been identified, but we know that inflammation is involved followed by fibrosis of the joint lining. This process sometimes follows some sort of injury to the joint but often occurs spontaneously, without any obvious provoking factors.
Frozen shoulder occurs more commonly in women than in men, tends to present in middle age, occurs in 1 in 5 diabetics, and can sometimes occur in both shoulders.
The good news is that the condition generally resolves or “thaws” spontaneously. The bad news is that this recovery can take from 6 months to more than 2 years. Furthermore, some patients report that their shoulder never recovers fully.
Fortunately, several treatment options are available that may ease the symptoms of this debilitating condition and even hasten the recovery to a full, pain-free range of motion.
In this article, we’ll explore the pros and cons of the most common treatment options ranked from least invasive to most invasive.
Physiotherapy
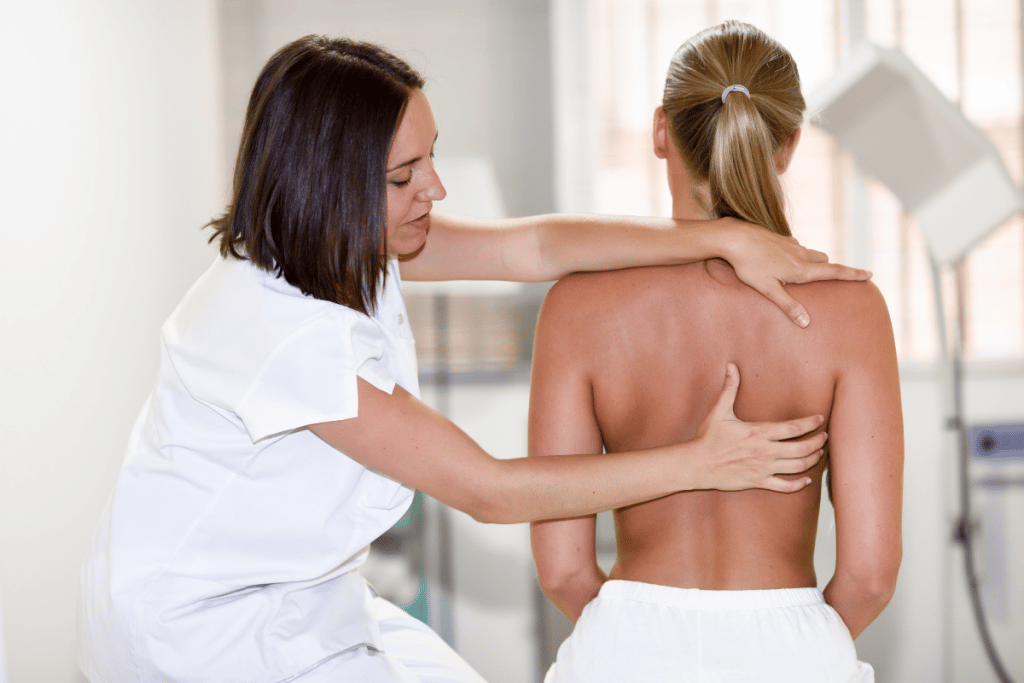
For most patients, enrolling in a physical therapy program is the key to recovery and should be considered the backbone of frozen shoulder treatment.
Patient education is one of the most vital components of the physiotherapist’s role. By gaining an understanding of their own condition and being made aware of their own progress, patients can manage their expectations, reduce their frustration and be more compliant with their home exercise programmes.
Physiotherapists will invariably employ some manual muscle release techniques, passive and active mobilisations and various stretches. Depending on the stage of the condition, the physiotherapist may choose to include dry needling, TENS machines or kinesiotherapy techniques.
Hot and cold therapy
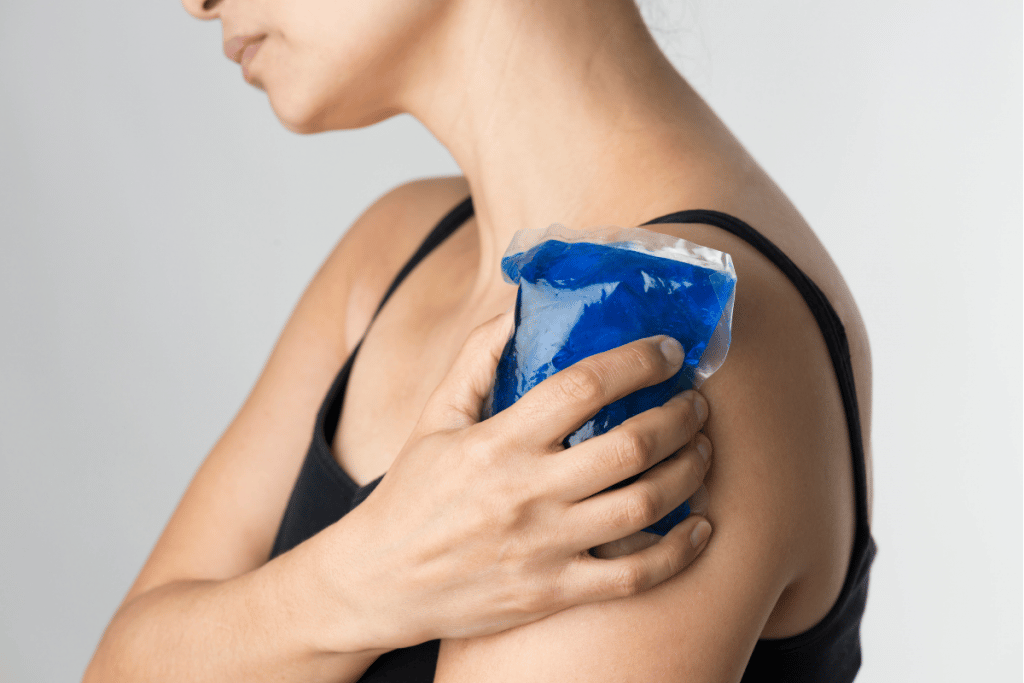
The joint is inflamed and painful during the initial “freezing stage” of frozen shoulder.
At this point, applying a heat pack might well make things worse. Choose a cold compress or ice pack instead to ease the pain.
In the later adhesive or “thawing” stages, heat packs can be very effective when used before a stretching or home exercise session to promote an increased range of motion.
Topical creams and lotions
Various warming and cooling gels are available over the counter. Although these ointments might feel pleasant or tingly when applied, they will not impart any significant benefit.
In the initial painful phase, gels and patches containing non-steroidal anti-inflammatory drugs (NSAIDs) such as diclofenac may help to ease pain and inflammation.
Oral medication
Doctors often prescribe non-steroidal anti-inflammatory drugs to Frozen Shoulder patients. However, there is no high-level evidence that confirms their effectiveness. Nevertheless, many patients report they do provide relief during painful phases.
Oral corticosteroids are also prescribed to patients with frozen shoulder. The drugs mimic cortisol, a hormone produced by the body to temper an overreactive immune response. Corticosteroids rapidly reduce inflammation either directly or throughout the body. Many patients report some improvement in function after their use.
Long term oral steroid use does run the risk of significant side effects and so these drugs should be used in short bursts, if at all.
Corticosteroid injections
By injecting a corticosteroid medication directly into the shoulder joint, the powerful anti-inflammatory effects of the steroid can be concentrated where they are needed most. If performed early in the disease process the degree of inflammation within the joint can be lessened leading to less severe fibrosis and fewer adhesions forming. For this reason, corticosteroid injections are considered more effective in the painful and freezing stage of the condition. The corticosteroid is almost always mixed with a local anaesthetic agent that will also reduce pain and aid with improving the motor control of the shoulder complex.
Success rates range from 44 to 80% and many patients report rapid pain relief and improved function within the first few weeks of the injection. The injection may be given at the sub-acromial site or as an intra-articular injection but a recent study suggested that combining both sites may be the most effective. Corticosteroid injection should be considered a first-line treatment for patients with pain as their predominant complaint in the early stages of frozen shoulder. By combining a corticosteroid injection with ongoing physiotherapy, patients may give themselves the best chance at a rapid recovery without the need for surgery.
Manipulation under anaesthesia (MUA)
This involves going to an operating theatre and undergoing a general or regional anaesthetic. Once anaesthetised, the surgeon forcefully moves the shoulder in all planes in an attempt to stretch and disrupt the capsule to regain range of motion. It is not without risk of complications such as dislocation or fractures or even nerve injuries.
MUA should be considered a last resort and reserved for patients who are resistant to physical therapy. After manipulation, an extensive post-manipulation programme is necessary to preserve any range of motion gained.
Hydrodilatation
Also known as distension arthrography, hydrodilatation has emerged as a potential non-surgical option in the management of frozen shoulder. It involves the injection of a large volume of fluid (usually containing some steroid and local anaesthetic) into the shoulder joint under x-ray guidance. The goal is to stretch and expand the joint capsule like a water balloon.
There is no high-level evidence to support the technique yet but some studies have shown that it can provide short-term pain relief and improved function for up to 3 months.
Arthroscopic capsular release
Open shoulder surgery is almost never performed for frozen shoulder anymore. Arthroscopic surgery or so-called “key-hole surgery” however, is a reliable and effective method for restoring range of motion in non-responsive patients. It allows a controlled release of tight capsular structures under direct vision and avoids many of the side effects associated with MUA (although nerve injuries remain a concern).
Arthroscopic treatment should be considered in patients unresponsive to at least 6 months of good conservative treatment.
Conclusion
When it comes to curing frozen shoulder quickly, we may need to redefine what we mean by “quickly”. Frozen shoulder is a condition that can grumble on for years and expectations of a “quick-fix” are unrealistic. That said, there are many treatment options available that can accelerate the journey to healing.
Early diagnosis is vital so that a corticosteroid injection has a chance to extinguish the inflammatory process. Ongoing physiotherapy can then restore any lost range of motion.
All hope is not lost for patients who fail to respond to conservative measures – more invasive treatments including MUA, hydrodilatation or arthroscopy can be effective at treating this frustrating condition.
By Dr. Jarrad Van Zuydam, Sports Physician
Take control of your shoulder recovery with Reflex Health
With Reflex Health monitor your shoulder range of motion and shoulder painShoulder pain is any pain felt around in and around the shoulder joint. The shoulder is the most mob More over time. Users say “It would be like going on a diet without tracking your weight loss.” Take control today by downloading the Reflex Health App.