AC Joint Injury can cover acute and degenerative causes. The AC joint stands of “Acriomion-Clavicular” joint.
What is the AC Joint?
The Acromion-Clavicular Joint (AC Joint) is the joint between the bony tip of the shoulder (acromion) and the collar bone (clavicle). The Acromion-clavicular joint is one of the synovial articulations of the shoulder complex which connects the axial to the appendicular skeleton.
The synovial joint is formed between the convex lateral clavicular and medial concave acromial ends.
A fibrocartilaginous disc similar to the knee’s meniscus sits between the articulating surfaces. Degeneration of this disc occurs with increasing age and activity and is thought to contribute to pain and disability in the elderly and overhead athletes.
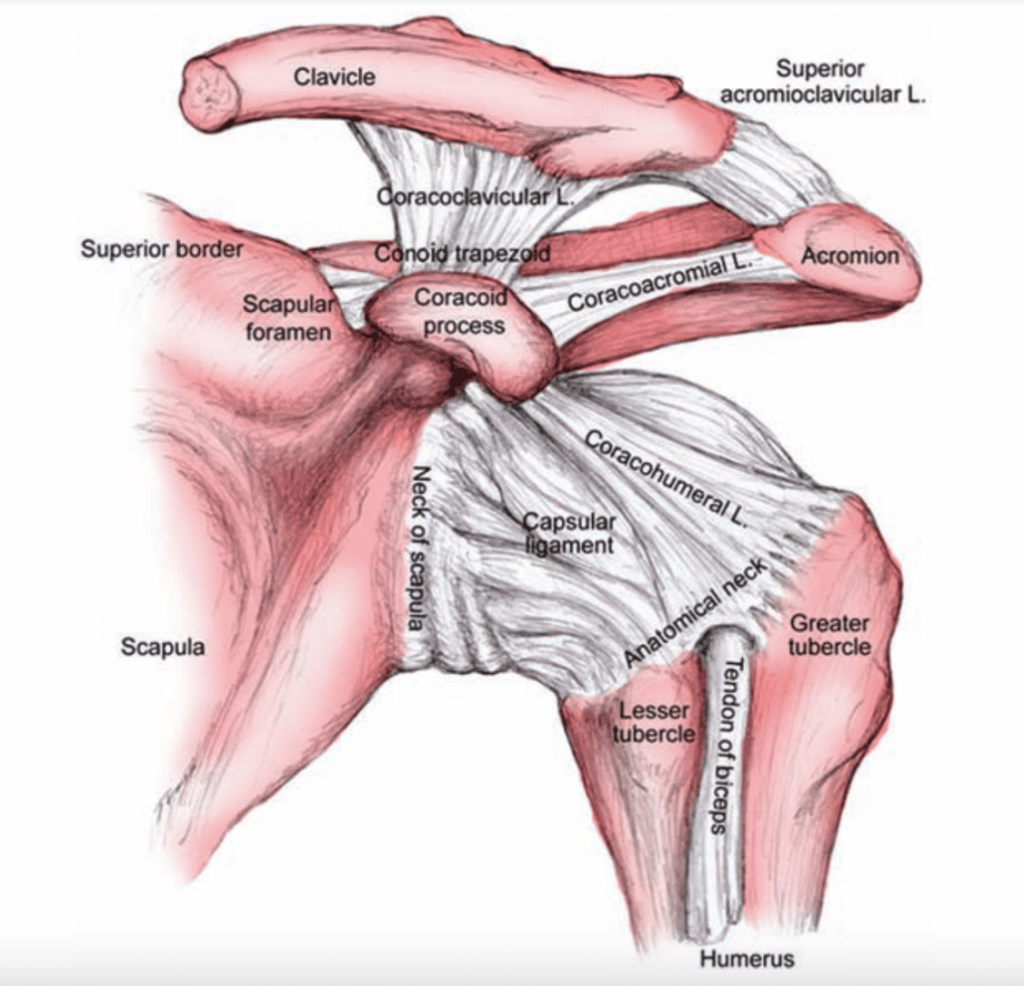
The AC joint has four planes of movement: anterior-posterior and superior-inferior.
The capsule surrounding the joint, the condensed acromioclavicular ligaments, and the coracoclavicular ligament complex is the restraint that keeps the joint in position and protects it from its dislocation.
AC joint injuries account for 9 to 12% of all shoulder injuries, both traumatic and degenerative injuries.
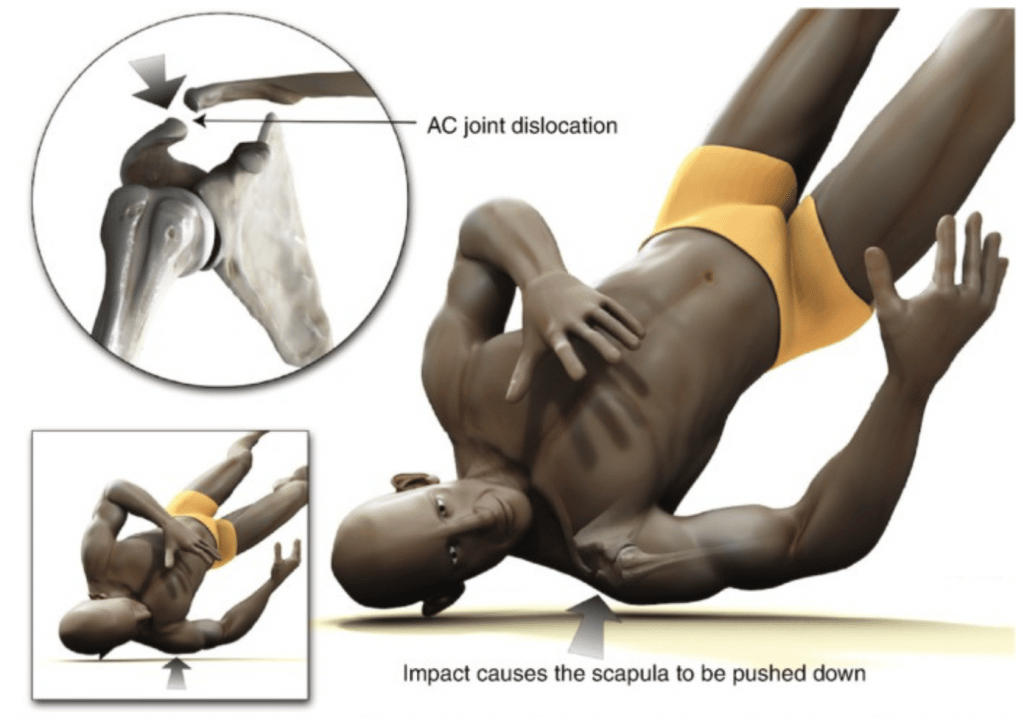
Traumatic AC injuries are mostly seen in people aged in the twenties whereas Degenerative AC Injuries are more prevalent in people in their fifties. The AC joint sprains which can be due to direct or indirect force are high in collision and combat sports like hockey, American football, rugby, and karate.
How to find the AC Joint?
The joint can be found by running your fingers along the clavicle, also known as the collar bone, towards the shoulder. At the point where the clavicle ends, depression can be sensed between the clavicle and an overriding acromion. This joint space is the AC joint space.
Can AC joint injury cause neck pain?
Yes, AC joint injuries can cause neck pain. The stability of the AC joint is provided by trapezius and deltoid muscles dynamically. They help in maintaining the joint position during movements of the arm. Hence any injury to the joint can cause a protective spasm in the upper trapezius and muscles surrounding the joint to guard the joint against further injury. Even some of the experimental pain studies have reproduced pain in the trapezius – supraspinatusThe supraspinatus is a muscle and tendon in the shoulder that connects the Shoulder blade (scapula) More, anterolateral neck region, and deltoid region by injecting saline in the AC joint.
AC joint can cause referred pain in the neck region, for which the joint needs to be tested clinical-radiologically, with good attention given to the mechanism of injury.
How do you treat an injured AC joint?
An injured AC joint is treated according to the mechanism of injury. A degenerative or a micro traumatic AC joint is de-loaded by activity modification or restriction, icing, and taping. The scapular muscles are strengthened statically and dynamically and flexibility is restored to normal length.
An acutely sprained AC joint is generally treated with rest and immobilisation in a sling. Mobility, motor control, and strength are built gradually as the pain settles down and movement becomes easier.
How long does the AC joint take to heal?
The healing of the AC joint depends upon the number of structures injured, the mechanism of injury, the intensity of the traumatic force, the age of the patient, and his/her occupational demands.
A degenerative joint disorder generally requires three to seven days of sling immobilisation with anti-inflammatories, physical therapy focuses on scapular control and flexibility, followed by activity modifications and strengthening. In some cases, intra-articular injections are also helpful in controlling inflammation.
Acute AC joint sprains are classified according to Rockwood classification, depending upon the ligaments and trapezius – deltoid fascia involved. Type 1 and 2 injuries are mild sprains without any separation of the joint surfaces. These injuries are treated non-operatively with rest, immobilisation in a sling a gradual physiotherapy program focussing on building strength and scapular kinematics. Depending upon the extent of the injury and other comorbidities it might take 3 to 12 weeks of rehabilitationRehabilitation is the process of helping a person regain strength and function after an injury. This More to heal an AC joint injury.
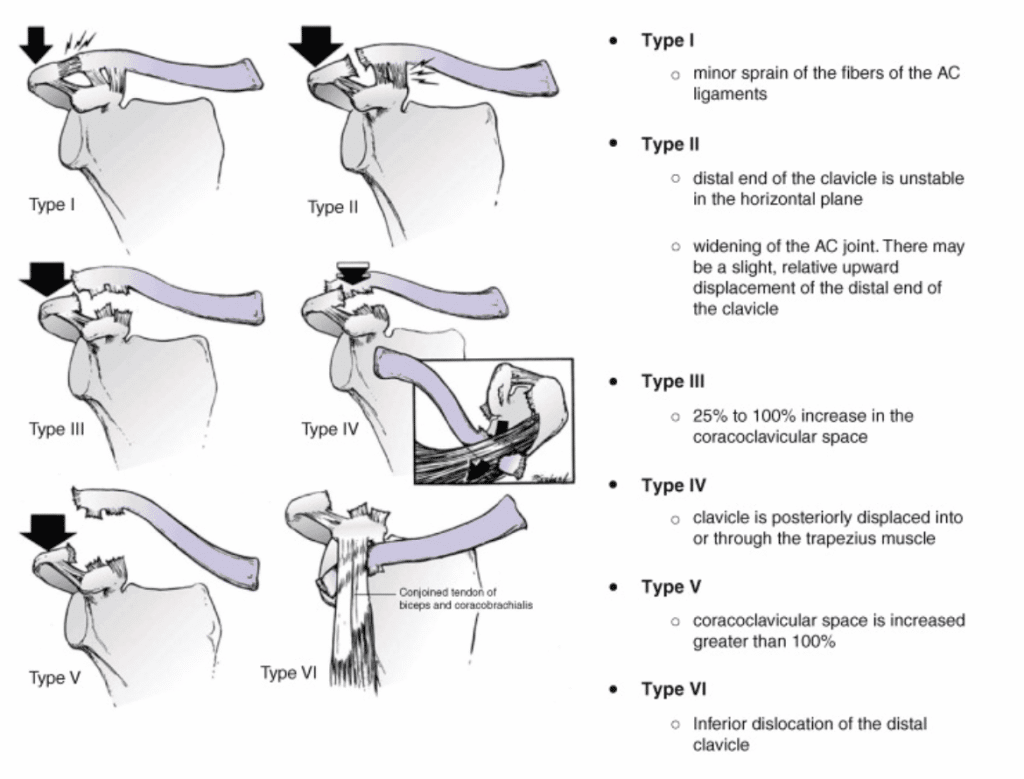
With respect to athletic injuries, especially in collision sports the player position, injury time compared to the athletic season, and throwing demands are taken into consideration to make treatment decisions. Athletes predisposed to further AC joint injuries are predominantly treated conservatively. Type 3 injuries can be treated both operatively and non-operatively depending upon the case and the structures involved.
Does AC joint separation need surgery?
Most AC joint separations are Types I- III and do not require surgery. Type IV – VI AC joint separations require surgery and can occur in high-impact traumas such as car crashes. These injuries have a high risk of instability of the shoulder jointThe glenohumeral joint is a ball-and-socket synovial joint and is the most mobile joint in the human More and are treated surgically with one of 4 types of procedures as follows:
- Primary repair of AC joint with pins, needles, or rods
- Distal clavicle resection and reconstruction of soft tissues(Weaver Dunn Procedure).
- Anatomic coracoclavicular reconstruction
- Arthroscopic fixation with sutures
The post-operative rehabilitation is gradual and might take 6 to 12 months for a full recovery and return to sport depending upon the structures involved and the surgical procedures used, with arthroscopic procedures requiring less time compared to the open ones.