The shoulder jointThe glenohumeral joint is a ball-and-socket synovial joint and is the most mobile joint in the human More is the most regularly dislocated joint in the body. It takes a strong force such as a blow to the shoulder to pull the bones out of place and cause a dislocated shoulder. Trauma from motor vehicle accidents and falls are also a common source of dislocation.
Patients with prior shoulder dislocation are more prone to redislocation as the tissues have not healed properly and the shoulder complex is weaker than normal.
Younger patients have a much higher frequency of redislocation; most likely due to higher activity levels.
What is a shoulder dislocation?
If you have a shoulder dislocation, it means that your upper arm bone (the humerus) has shifted out from its normal position in the shoulder joint.
Medically, a dislocation is defined as a total loss of contact between the two ends of bones .
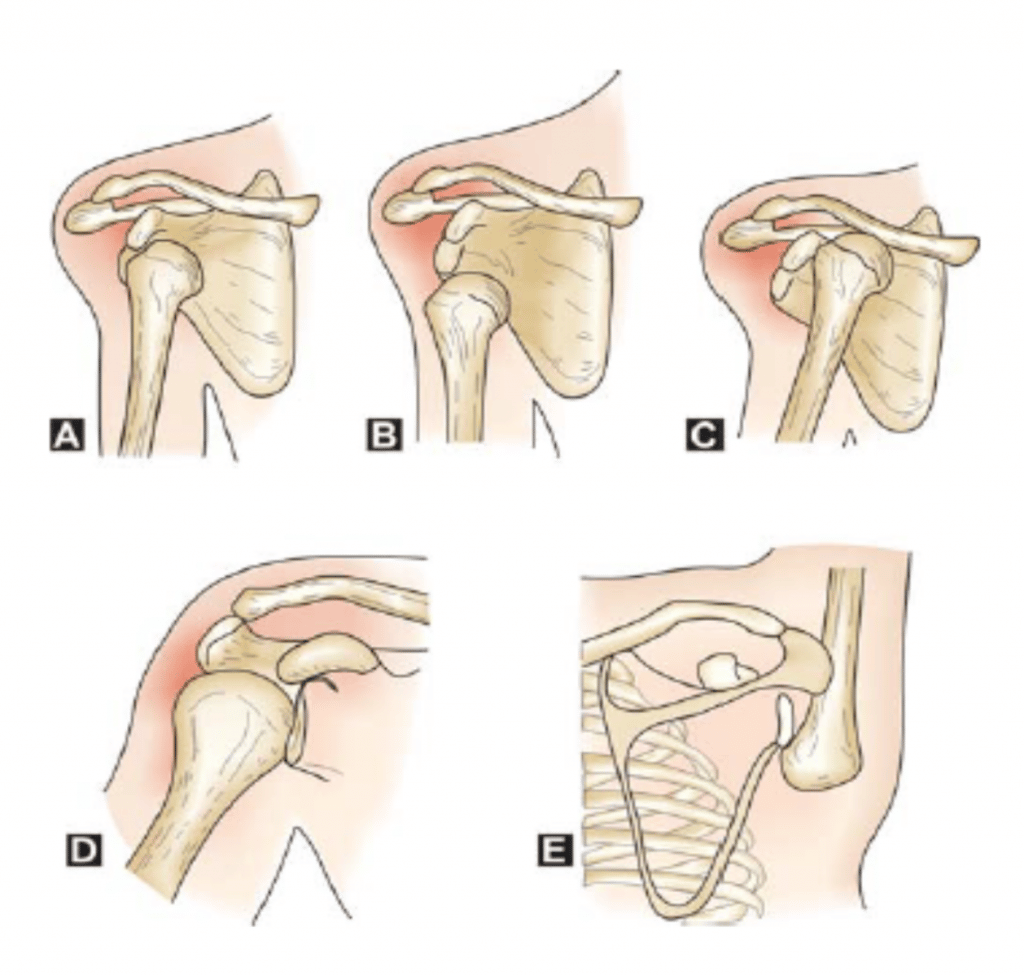
What are the 3 types of shoulder dislocations?The shoulder can dislocate in three directions:
- Anterior dislocation (forwards)
- Posterior dislocation (backwards)
- Inferior dislocation (downwards)
- The most common dislocation is the anterior dislocation, accounting for up to 97% of the cases.
ICD 10 – Shoulder dislocation
The World Health Organisation (WHO) published the ICD-10 which stands for International Classification of Diseases. Medical terms are coded according to ICD form the main basis for health recording and statistics on disease in a primary, secondary, and tertiary care.
In the ICD 10 codes, S40-S49 represent injuries to the shoulder and upper arm.
Out of these codes, S43 is a code indicative of subluxation or dislocation of the shoulder joint. To enable the assignment of correct ICD-10 codes, the documentation ideally specifies the positioning, location of the dislocation including laterality (right or left), joint involved, the extent of the dislocation, and encounter.
However, a note must be made that the ICD-11, was adopted by the 72nd World Health Assembly in 2019 and came into effect on 1st January 2022.
Treatment for a Dislocated Shoulder
The treatment for shoulder dislocations depends on the patient’s age, symptoms, the severity of dislocation, patient’s level of fitness, and patient’s goals.
Both conservative (non-surgical) and surgical management are options for treating shoulder dislocation, which attempts to restore a fully functional, pain-free, and stable shoulder. Closed reduction of the dislocation is generally performed before conservative or surgical treatment.
(closed= the surgeon won’t cut your shoulder open, reduction=put your shoulder back in place). Which is then followed by physiotherapy and a rehabilitationRehabilitation is the process of helping a person regain strength and function after an injury. This More regimen.
However, if the dislocations are severe and recurrent, there is no role of conservative management. Operative care may entail open or arthroscopic surgery and is typically followed by a monitored physical therapy programme.
How long does a dislocated shoulder take to heal?
- After a closed reduction under general anaesthesia is done, the shoulder is immobilized in a sling.
- Ideally, the immobilization period is for 3 to 6 weeks.
- However, this can depend on a plethora of factors namely- age, presence of co-morbidities like diabetes, addictions like smoking, etc. that can delay wound healing.
Dislocated Shoulder Range of Motion
If you are, let’s say, at the gym and hear your shoulder pop out, – do not try to stretch it, do not apply traction, do not rotate, twist, or turn the shoulder.
Shoulder dislocations can be associated with labral tears (labrum = a thick layer of tissue around your shoulder joint that keeps the joint intact), rotator cuffThe rotator cuff is a group of muscles and tendons that attach the shoulder blade to the upper arm b More injury (the shoulder muscles you were probably trying to strengthen in the gym when this pop occurred), humeral fractures (humerus = the upper arm bone), nerve damage, etc.
All of these associated injuries don’t always happen, but you will not know that until you visit a healthcare professional.
How long does it take to get the full range of motion with a dislocated shoulder?
There is no one correct answer for this. Multiple patient factors govern the treatment plan and also determine the time it would take to gain the full range of motion (ROM) back.
For a young healthy active adult who was treated non-operatively,
- Phase 1 (up to 6 weeks)
Since the shoulder is in a sling, the focus is on the elbow, wrist, and finger ROM. Gentle strengthening without movement (isometric) exercises for the muscles around the shoulder can be started towards the end of this.
- Phase 2 (6-12 weeks)
Ideally, this is the time when the full ROM of the shoulder should return to normal. Strengthening of the shoulder muscles can be started depending upon the patient’s symptoms and wound-healing capacity.
- Phase 3 (12- 24 weeks)
A high level of exercise (plyometric) training can be started for athletes wanting to return to sports.